Biliary Atresia
Key points
- Biliary atresia is a rare condition in babies
- The first sign of biliary atresia is usually yellowing (jaundice) of the skin at about 2 to 6 weeks of age
- It happens when the bile ducts inside or outside the liver are blocked by scar tissue
- Bile builds up in the liver and damages it
- This stops the liver from working properly and leads to scarring and cirrhosis
- There is no cure for biliary atresia, but it can be treated with surgery or a liver transplant
- Children with biliary atresia must usually follow a special diet all their life
Transcript
Veronica: It was a complete shock when we got into that fifth week and we did the biopsy and it came Biliary Atresia, and the same day the doctor came and said, okay, we’ll do the operation tomorrow, my husband and I were…
It’s a life-threatening, you know, illness, it’s a lot to take in. There’s no option, there was no option, so, yeah it was an experience.
Morgan: Well I’m in year six and I like drawing I like the movies and I like roller skating and I also like playing netball and hanging out with my friends.
Veronica: We had a paediatrician came to see her and then, when she saw how yellow she was and the blood test, she said look it could be nothing, or it could be Biliary Atresia. It’s very rare.
Biliary Atresia, what it is in simple terms, is the bile ducts that they are, we have inside the liver and outside the liver, some of those ducts, or they are fibrosis, so sort of they don’t exist or they’re blocked, and your bile doesn’t flow through your system.
So, we did the biopsy and then the doctor came to see us, we have an opening for tomorrow, and we were first parents, it’s just a bit of a shock. She was only six weeks old. So then they put us, they would say yes, we need to do it, so they did this procedure; was around eight, ten hours operation. Success. I remember one of the things that show you if it’s success or not is the colour of the poo, and it was normal. This operation, the idea is that if it’s successful you can extend the life of the liver you’ve got and then it gives you more time to grow and get a better liver later in life.
Between eight and nine we noticed quite a bit of a decline and the doctors the same. You get sort of water inside your belly and that makes that your belly becomes bigger and bigger with time.
Morgan: Well no one at my school could really tell. It was kind of hard for clothes to fit because, like, there’s a big ball on my belly.
Veronica: The other things that I could notice obviously were energy levels in comparison to other kids you will see kids running, running, running; she was sitting drawing.
Then it was decided to put her in a transplant list. Before we can put in a transplant you have to visit quite a few doctors and do lots of tests, so we spent quite a bit of time in hospital the year of the transplant. And then once going onto the list we were lucky enough that within a month we got the call – transplant. It was in the middle of the night, around 11, that we need to be in hospital around five in the morning. We woke up Morgan – ‘Morgan, do you want to come?’ – but then she realised, yep, I want to come, I’m ready.
And then we go to hospital they do all the preps, and then ready for the operation room.
Morgan: My dad put on this silly cap.
Veronica: Yeah, we all put the silly caps on and there was lots of people, lots of machines, and we have to give her a kiss until she went to sleep. And then I think the operation lasted around 12 hours or so.
To see her, she was connected, so it’s quite a big shock when you see your kid connected to a lot of things.
Morgan: So I got out of bed after my operation and I told mom that this is what it feels like to be alive.
Veronica: So she spent 10 days in ICU and about a couple of weeks, a bit less, in in a ward.
Morgan: And then I got to leave on my birthday.
Veronica: That’s right, yeah, that’s right.
Morgan: Oh yeah, well all the teachers at school said, ‘Are you okay, honey you look so different…’
Veronica: Her face changed completely.
Morgan: Yeah, they like I would like now like yesterday I was running around we were playing tag and it was really fun, so, yeah, I did notice a bit. Yeah, when I left hospital I had a lot of medicine.
Veronica: We are almost two years after and we just with one medication, which is the anti-rejection medication. It seems like it was not that long ago, but it feels really far away, which is a good thing.
My advice to other families or kids with Biliary Atresia will be to first follow the doctor’s advice to the T – so take the medications when they need to be taken, follow exactly what they said, and for the kids just be yourself, it’s not much different than any other kid and everything will get there at the end.
Morgan: My advice is to not worry about it because the doctors know what they’re doing, and that you just need to trust the process.
Transcript
Biliary Atresia is a rare liver disease that occurs in babies. It is present in about one in 14,000 live births, so that gives you an idea of how rare it is. The disease is thought to start while the baby is still inside the mother’s womb and it involves a progressive damage, inflammation and scarring and blockage of the bile ducts in the liver.
The bile ducts are very important because the liver makes bile and the bile ducts are the tubes through which that bile is transported to the gut, where it’s important for breaking down fat and helping you absorb vitamins. If the bile ducts are blocked, which they usually are by the time the baby is born, the baby will present with jaundice, look yellow because the bile can’t get out of the liver. The bile that’s in the liver will cause progressive damage to the liver and because the bile is not reaching the gut where it should be, the baby can’t absorb fat properly, so it doesn’t grow and isn’t able to absorb many of the important vitamins; that can cause problems with bleeding and bones, mineralisation and lots of other issues.
The cause of Biliary Atresia is not known. We don’t really know who gets it or why. There are some theories about an infection followed by some sort of uncontrolled inflammatory process that isn’t able to stop. There is much research around the world trying to find the cause of Biliary Atresia, but as yet unfortunately nobody knows.
Because Biliary Atresia is not an inherited condition, we know from research all around the world that if you do have a baby with Biliary Atresia, you are almost certainly not going to have another child with Biliary Atresia.
Biliary Atresia, because it presents very early after birth with a baby with jaundice, that’s usually the first clue that there is something wrong. So if the baby is jaundiced, a blood test is done to show what type of jaundice it is, followed by some tests including an ultrasound and perhaps a biopsy of the liver. That’s where we take a little small sample through a needle of the liver and look under the microscope at it. Sometimes we have to do a special x-ray called a cholangiogram and together these pieces of information will help us diagnose Biliary Atresia.
The treatment for Biliary Atresia is somewhat urgent. We need to diagnose and treat it as soon as possible. Once the diagnosis is made, hopefully within a few weeks of life, the first treatment is a special operation called a Kasai operation, which was developed in Japan in the late sixties.
The operation involves removing the damaged bile ducts and connecting a loop of bowel to the liver, with the hope that some of the bile ducts that are still in the liver and open will allow bile to drain into the gut.
This operation works reasonably well in about 50% of children. In the group of children where it doesn’t work, they are likely to need a liver transplant within the next year or two of life. In the children where it does work, that can enable them to grow and go to school and lead a reasonably healthy life, but we know that most children with Biliary Atresia will need a liver transplant before they reach adulthood.
Apart from the liver transplantation and while the child is growing, we will supplement the child with special feeds to enable them to grow and multiple types of vitamins to prevent bleeding and to allow bone growth and eye development, etc.
Life with a baby with Biliary Atresia is difficult and it’s quite challenging. It does involve being closely attached to a fairly major hospital with paediatric gastroenterologists and other specialists who will help manage the child. There may be additional feeds required at home, special formulas, or sometimes if the baby’s not drinking well, we need to put a little tube through the and into the stomach and feed the baby through that tube.
This difficult journey has been travelled by many, many families, so there’s a lot of information and a lot of resources and support out there for families with Biliary Atresia.
I would suggest the Liver Foundation website has information on Biliary Atresia. There’s also information available on parent support groups of which there are some in Australia and the US and there are also some multi-centre collaborations both in Europe and in America.
What is biliary atresia?
Biliary atresia is a condition that affects the bile ducts. These are tubes that that carry bile out of the liver. Bile is a liquid that the liver puts out to carry away waste and help the body digest fats and vitamins.
If your baby has biliary atresia, they may have been born with no bile ducts, or the bile ducts are blocked or inflamed.
Soon after birth, the bile starts to build up in the liver. Here the bile quickly starts to destroy liver cells. This causes scarring of the liver and cirrhosis.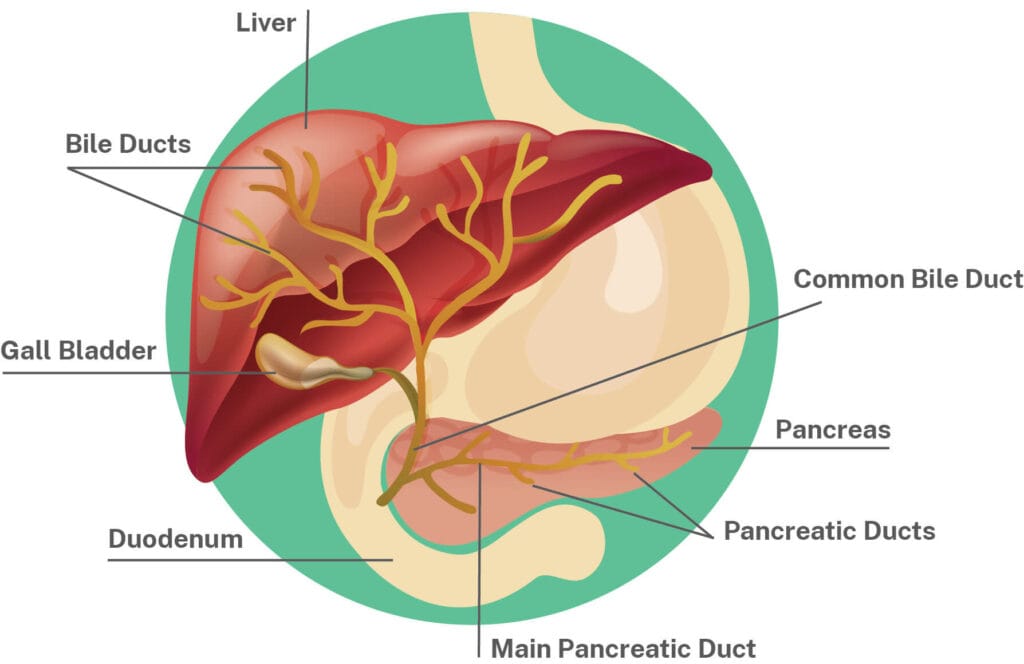
What are the symptoms of biliary atresia?
The symptoms of biliary atresia normally come on around 2 to 6 weeks after birth.
The first sign is often jaundice, or yellowing of the skin and whites of the eyes. This is caused by too much of the substance bilirubin in the blood. It’s a sign the liver isn’t working properly.
Jaundice is common in newborn babies. But if it first starts between 2 and 6 weeks of age, and doesn’t clear up in 1 to 2 weeks, it might be a sign of biliary atresia.
Other signs and symptoms of biliary atresia are:
- A swollen belly
- The liver feels hard
- Pale grey poos (that look like clay)
- Dark yellow or brown urine
- Feeding more often.
Read more about the symptoms of liver disease
How is biliary atresia diagnosed?
There are lots of conditions that can cause the symptoms above. To confirm biliary atresia, your doctor will order a range of tests. These tests are often done in a children’s hospital.
Tests your baby may need include:
- Blood tests to check how well the liver is working
- Urine tests
- An ultrasound to look at the shape and size of the liver
- Tests to see how the bile is flowing through the liver (nuclear medicine scan or cholangiogram)
- A liver biopsy, when small piece of liver tissue is removed with a needle and then looked at under a microscope.
Why does my baby have biliary atresia?
Biliary atresia is only found in newborn babies. It is very rare. Worldwide, only about 1 in every 15,000 to 18,000 babies is born with biliary atresia.
We don’t fully understand why some babies are born this way. There is some evidence biliary atresia may be caused by a virus or an autoimmune condition (when the body’s immune system goes into overdrive). It doesn’t seem to be caused by genetics and you can’t catch it from someone else.
Babies born with biliary atresia often also have abnormalities in other organs like the heart, kidneys or spleen.
How is biliary atresia treated?
There is no cure for biliary atresia.
The main treatment is surgery. The surgeon removes the gall bladder and the damaged bile duct outside the liver. They connect the liver straight to the small intestine to drain the bile from the remaining bile ducts in the liver. This operation means the bile can flow out of the liver again and the baby’s jaundice and other symptoms disappear in a few weeks.
The surgery is called the Kasai procedure or a portoenterostomy. It needs to be done as soon as possible, and before 3 months of age.
What to expect from surgery
Your baby won’t be able to feed for a few hours before the operation. They will have a drip inserted to give fluids and then they will be given a general anaesthetic to put them to sleep. The surgery will last for several hours.
Afterwards your baby will need several medications such as antibiotics and pain relief. They will have drains from their stomach and bladder. They will need further tests to make sure the liver is working properly.
Your baby won’t be able to feed for up to 72 hours after surgery, to give the bowel time to heal. They will be fed through a tube going from their nose to their stomach (naso-gastric tube).
The surgery is completely successful in about 1 in 4 cases. In half of cases, the bile will flow but not very well.
In the other 1 in 4 cases, there will be no bile flow even after surgery. Sometimes the problem is with bile ducts inside the liver itself. In these cases, the only possible treatment is a liver transplant.
If your baby needs a liver transplant, it’s important that it’s done as quickly as possible – before too much damage has been done to the liver.
Read more about liver treatmentsCaring for a baby with biliary atresia
You may be able to breastfeed your baby, but many babies with biliary atresia also need a special milk formula that contains fats that are easier to digest and help them gain weight.
If the surgery is completely successful and the bile is flowing well, your baby can grow up normally. They will be able to eat a normal diet.
If your child can’t absorb fats or vitamins properly, they will need to eat a special low-fat diet and take vitamin supplements. The most common supplements are vitamins A, D, E and K.
If your child has a special eating plan and still doesn’t grow properly, they may need a feeding tube (naso-gastric tube) to take a high calorie supplement straight into the stomach. Sometimes children with biliary atresia need to be feed through a drip (intravenous line).
There are some complications or biliary atresia to watch for:
- Cholangitis: Cholangitis is an infection of the bile ducts caused by bacteria. This is a common problem after surgery and can be life threatening. Seek medical help straight away if your baby has had surgery for biliary atresia and develops a fever, the jaundice gets worse, they’re not eating, or they’re more irritable than normal.
- Cirrhosis: Biliary atresia can cause long-term damage to the liver, called cirrhosis. This stops the liver from working properly and can affect the growth and physical development of the child.
- Failure to thrive: If the bile isn’t getting to the small intestine, the child can’t absorb their food properly. This can lead to poor growth or vitamin deficiencies.
- Portal hypertension: This is pressure on the veins travelling through the liver. It is caused by the scarring. Increased pressure on the portal vein can cause an enlarged spleen, ascites or varices.
- Ascites: This is a build-up of fluid, causing the child’s tummy to swell up.
- Varices: Varices are enlarged veins in the food pipe or stomach that can burst and cause internal bleeding. The signs of bleeding might be blood in the vomit or very dark or black poos. If you notice these symptoms, take your child to hospital straight away.
What is the outlook for a baby with biliary atresia?
The chances of long-term survival from biliary atresia are excellent in Australia. But if it’s not treated, biliary atresia usually leads to death by age 2.
If the surgery is successful, children may go on to lead a normal, healthy life. But in most cases, the liver still gets gradually damaged over time. Children born with biliary atresia often go on to need a liver transplant later in childhood or as a young adult. Biliary atresia is one of the main reasons children have liver transplants in Australia.
All babies born with biliary atresia will need to be monitored closely throughout their lives. Their growth and nutrition will be regularly checked and the specialist team will look out for possible complications.
Additional information and support
- Rare Voices Australia
- Australian Clinical Trials
- Children’s Liver Disease Foundation (UK)
- National Organization for Rare Disorders
What next?
References
American Liver Foundation. Biliary Atresia
Children’s Liver Disease Foundation. Biliary atresia
National Institute of Diabetes and Digestive and Kidney Diseases. Biliary Atresia
National Organization for Rare Disorders. Biliary atresia
Russo P, Rand EB, Loomes KM. Chapter 10: Diseases of the biliary tree. In: Russo P, Ruchelli ED, Piccoli DA, eds. Pathology of Pediatric Gastrointestinal and Liver Disease. 2nd ed. Berlin: Springer-Verlag; 2014;395–444.
Song W, Sun LY, Zhu ZJ, Wei L, Qu W, Zeng ZG, Yang YS. Characteristics of Gut Microbiota in Children With Biliary Atresia After Liver Transplantation. Front Physiol. 2021 Jun 29;12:704313. doi: 10.3389/fphys.2021.704313. PMID: 34262484; PMCID: PMC8273867
The Sydney Children’s Hospitals Network. Biliary Atresia
Reviewed November 2022
