Primary Biliary Cholangitis
Key points
- Primary Biliary Cholangitis (PBC) is a rare condition that affects the small bile ducts (the network of small tubes that carry bile in the liver)
- Over time, the bile ducts can become inflamed and scarred
- PBC may eventually lead to long-term liver damage and liver failure
- If treatment is started early, the outcome can be excellent
- Without treatment, the condition is likely to get worse
- Some people have disease that responds poorly to treatment and may need a liver transplant
Transcript
I’d been having annual blood tests for cholesterol and liver function for years and it just so happened that I hadn’t been for a while.
So next time I saw my regular GP, I said to him ‘Look we probably need to do one of these tests’.
And I said to one of my closest friends – I don’t know why I said – ‘I don’t think I want these results’.
And I got a phone call from my GP, which was really unusual, and he said ‘Look, I need to see you and I need to see you soon’.
And I said, ‘Don’t play around, something is obviously wrong, what’s going on?’
And he said to me, ‘Look, your liver function’s really high I need you to go see a specialist.’
And when I went in there, he was somebody I knew quite well, and he kind of said, ‘What are you doing here?’ and I said, ‘Look at my bloods.’
And he saw how high they went, and we both kind of thought it was fatty liver. And he asked me to have a whole bunch more tests, which I did.
And he said to me ‘I’ve got something important to tell you, it’s really serious.’
And then he started giving me a whole lot of the detail and I just kind of went, ‘Stop, I feel overwhelmed with the detail, just give me the headlines.’
And he did, and he wanted to give me some information to go and read up.
And I said, ‘Look, you know I know myself, I would prefer to tackle that.’ Because I then had to have a biopsy for them to stage it. I said, ‘When I’m ready I’ll have a look at it, but I don’t want to live in a space of fear, well I don’t know what I don’t know.’
So we arranged the biopsy and when it was done and then I went to get the results to what stage it was at and I just saw him gulp and I thought, ‘Shh, that’s not good.’
And he said it was like late stage 3 early stage 4.
Now I have to say I did not have any symptoms, so I felt well. The only thing I had was a bit of long bone pain. And he looked at me and he said with such intensity and care, ‘This is my area, I will see you through this.’
When I was having a follow-up session with my specialist, he mentioned the fact that there was the potential for a trial. And honestly, as far as I was concerned, anything that was going to help I was there for.
And they nominated a clinical trial co-ordinator and I was like a heat seeking missile – ‘What’s happening? When’s it going to come?’ Because there was a real question as to whether it would come to Australia or not, and it did.
And when I finally got the call that I was in and that it was happening I was delighted because there were so few things at that point that had real efficacy with PBC, so whatever it took I was signing up for I honestly cannot tell you the level of gratitude I have for that trial.
There are moments of worry, I cannot lie, that when I have blood tests is going to show elevation, but it’s not an unmanageable stress about it, it’s just this is what it is – and my life really isn’t any different on a day-to-day basis.
If you are overwhelmed and you’re asking for help, there lots of tools available, and a big one is the Liver Foundation.
And I encourage you to use whatever is available.
There – and that’s the diagnosis story.
Transcript
PBC is a rare medical condition. PBC stands for primary biliary cholangitis. It’s a medical condition that affects the small bile ducts in the liver.
These are little tubes that drain the bile from the liver into the main bile duct. Over a period of time, the liver disease impacts on the bile ducts by causing inflammation and scarring called fibrosis and eventually, if untreated, this may lead to more severe fibrosis or scarring and cirrhosis of the liver.
PBC is an autoimmune liver condition whereby the body’s own healthy immune system becomes overactive and attacks healthy liver cells and liver tissue. We do not understand why the immune system is fully activated to attack the liver in this manner. It is thought that we inherit genes that predispose us to this medical condition.
These genes may be activated by environmental triggers such as urinary tract infections, smoking and even certain chemical exposures, although that is not fully understood.
Most people are not aware they have PBC and do not have symptoms. It is often picked up incidentally when one goes to the doctor and has blood tests for an unrelated medical condition. The doctor may then look at doing further blood tests such as autoimmune blood tests and autoantibodies to try and clarify that you do have PBC. They may then go on to as well order certain scans such as an ultrasound, a Fibroscan or other more sophisticated imaging of the bile ducts to make sure you do not have another condition that can present in a similar way.
Sometimes it is necessary to have a liver biopsy to clarify that you do have PBC and you don’t have some other autoimmune liver condition.
The mainstay of treatment is a medication called ursodeoxycholic acid which is a derivative of a bile salt that we make in our own bodies that is a healthy bile salt. It is a well-tolerated medication, and most people will be prescribed this long term.
If you do not respond to this treatment or one of the rare people who do not tolerate the treatment we now have available on the PBS authorisation a medication called obeticholic acid. This is a good addition to the ursodeoxycholic acid and will treat more people.
In addition, we sometimes use a cholesterol lowering agent called fenofibrate or similar. This drug is used in combination with ursodeoxycholic acid and obeticholic acid.
I would like to emphasise as well there are newer drugs completing phase three clinical trials, which gives a bright future for this medical condition and these medications should become available in the next few years.
Most people with PBC have a very good outcome if they have ongoing regular treatment. Some patients, however, do not respond to treatment and will develop complications. This is a consequence of scarring of the liver bile ducts, which we call fibrosis, and this may lead to cirrhosis. Those people may need to have a liver transplant if they develop liver failure.
Other more common complications that can occur on a day-to-day basis include significant tiredness and fatigue. It is very important that you first of all go and discuss this with your doctor to make sure you’re optimising your health, you’re receiving adequate rest, diet and exercise and appropriate supplements.
Other complications that can occur are an elevated cholesterol that can lead to its own complications and osteoporosis, or brittle bones. Both of these conditions have medications that are easily accessible and you can receive those and get good treatment.
Some patients develop a profound itch, and that is a little bit more complicated to treat, but you need to discuss that with your doctor and pharmacist so you can receive appropriate treatment.
Other people develop a fluid overload, where they retain fluid and develop swollen legs and ankles or a swollen belly, and there are medications for this. So again it is important that you discuss this with your GP or specialist.
I would encourage people who are diagnosed with PBC to think in a very positive manner. There are good medications, there’s increasing availability of newer medications, and we are very good at treating the complications of a condition today.
So I would encourage you to engage your medical practitioners and make best use of their knowledge to have a positive outlook on your condition.
What is PBC?
Primary Biliary Cholangitis (PBC) is thought to be an autoimmune disease. That means the body’s own immune system attacks healthy cells and tissue.
If you have PBC, your immune system starts to attack the small bile ducts. The ducts get inflamed and blocked. Eventually, they are destroyed. If this happens, bile builds up and causes liver damage.
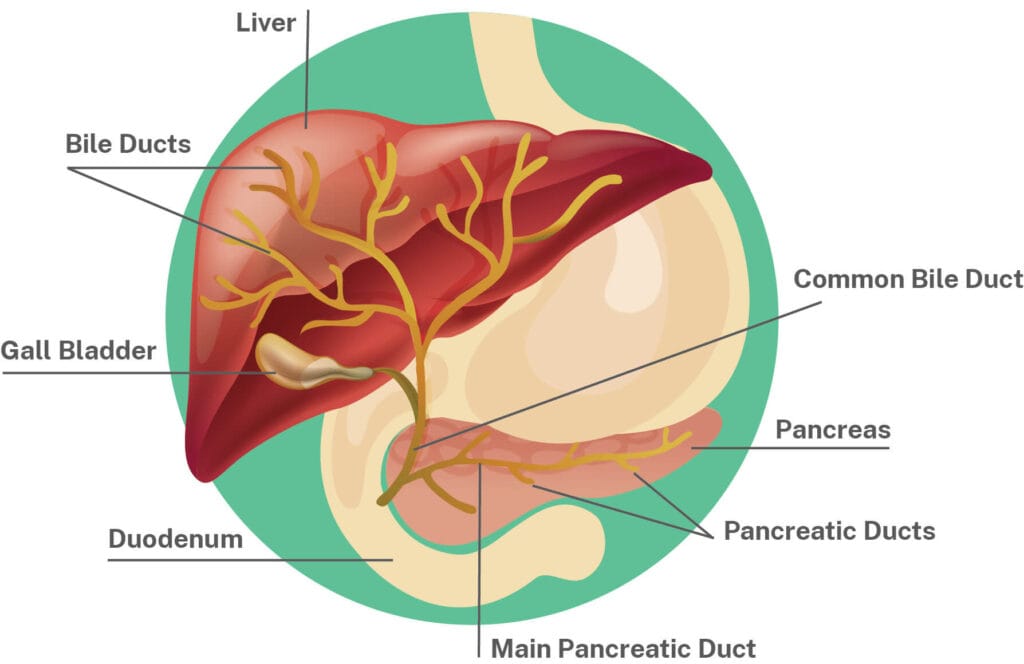 PBC is a chronic disease (it lasts for a long time) and without treatment it gradually gets worse. Over 15 to 20 years, someone with PBC can slowly develop liver failure.
PBC is a chronic disease (it lasts for a long time) and without treatment it gradually gets worse. Over 15 to 20 years, someone with PBC can slowly develop liver failure.
Although PBC is a very rare disease, the number of people who have it is increasing in Australia. Almost all of them (95%) are in women aged 35 to 70. It’s most common in middle age, between 45 and 65.
PBC used be called Primary Biliary Cirrhosis.
What are the symptoms of PBC?
PBC often doesn’t cause any symptoms. People only find out they have PBC because they have a blood test for something else.
If you do have symptoms, they usually start with feeling very tired (fatigue) and having itchy skin.
As the PBC gets worse, other symptoms may start. These include:
- Dry eyes and mouth
- Small yellow or white bumps around the eyes, eyelids, palms, soles, elbows or knees (these are deposits of cholesterol)
- Diarrhoea or oily poos because the body can’t digest fat properly
- Swollen feet and ankles
- Swollen belly due to build-up of fluid
- Darkening of the skin
- Enlarged liver or spleen
- Weight loss
- Yellowing of the skin and eyes (jaundice). This is a sign the disease is quite advanced
- Pain in the upper right of the belly
- Pain in the joints, muscles or bones.
PBC can also cause other problems such as:
- Liver scarring (cirrhosis)
- Osteoporosis (brittle bones)
- Portal hypertension – the portal vein is the main blood vessel that carries blood into the liver. When blood can’t flow into the liver, pressure builds up in the vein. To relieve pressure in the portal vein, the blood takes detours around the liver in other veins in the oesophagus (food pipe) or stomach. This condition can lead to swelling of the belly (ascites) as fluid leaks out of the of the liver, or swelling in other veins (varices). When veins get swollen, they can burst and bleed, which can be life threatening
- Gallstones or bile duct stones
- High cholesterol
- Underactive thyroid
- Vitamin deficiency (your body can’t absorb vitamins including A, D, E and K)
- Problems with memory and concentration.
How is PBC diagnosed?
 If your doctor thinks you may have PBC, they will order some blood tests to check for signs of liver disease or injury to the bile ducts. The blood will also be checked for antibodies that signal you may have PBC. These are called antimitochondrial antibodies (AMA). You will probably also have a cholesterol test.
If your doctor thinks you may have PBC, they will order some blood tests to check for signs of liver disease or injury to the bile ducts. The blood will also be checked for antibodies that signal you may have PBC. These are called antimitochondrial antibodies (AMA). You will probably also have a cholesterol test.
Some people may also need an ultrasound, FibroScan or other imaging to look at the bile ducts and rule out other diseases that have similar symptoms.
If it’s still not clear what’s causing the disease, you may need a liver biopsy. This is when a small piece of tissue is removed from the liver to be examined under a microscope.
It’s recommended that people with PBC are also checked for other autoimmune diseases such as coeliac disease, thyroid disease and Sjögren’s syndrome.
Read more about liver testsWhy did I get PBC?
We don’t fully understand what triggers the body to turn against its own cells. It’s possible that you inherit genes from your family, or that something in your life caused it to happen. Some of the triggers for PBC are thought to be:
- Smoking
- Exposure to some chemicals
- Urinary tract infections.
How is PBC treated?
There’s no cure for PBC, but medications can be used to slow it down and prevent complications. These medicines can make some people even more itchy, others have less side effects. Your doctor will help you decide what is the best treatment for your personal circumstances.
Medicines you might be given include:
First line treatment:
Ursodeoxycholic acid or UDCA capsules help the liver work properly by moving bile out of the liver and into the small intestine. This medication can prevent the PBC developing into liver failure. You will need to take it every day for the rest of your life
Second line treatments:
For people who don’t improve with or can’t tolerate UCDA, second line treatments are available.
Obeticholic acid is available on the PBS and can be used in combination with UDCA if you haven’t responded well to it, or as monotherapy (the only medicine) if you have had a reaction to UDCA. However this medicine is contraindicated (not safe to take) in people with cirrhosis and features of liver failure such as jaundice or fluid in the belly. It can cause worsening of itch, so is not recommended in people with itching as a problem.
Elafibranor is a new medicine that has been approved by the TGA for second line treatment of PBC and is usually used in combination with UDCA, but can be used by itself if UDCA is not tolerated. It is now available on the PBS. It is not associated with worsening of itch.
Seledelpar is another new medicine that has been approved by the TGA for second line treatment of PBC and is usually used in combination with UDCA, but can be used by itself if UDCA is not tolerated. It is not yet listed on the PBS.
Fibrates (fenofibrate and bezafibrate) have been used to treat people with and inadequate response to UDCA and they are effective, however neither medicine is approved in Australia for the treatment of PBC.
There are also treatments for some of the complications of PBC. Your doctor might give you medicine to treat high cholesterol, osteoporosis or portal hypertension. You will need regular liver function checks. If you start to develop liver cirrhosis, this will also need to be treated.
Eventually, the PBC can lead to liver failure. Having a liver transplant is usually very successful. Sometimes the PBC can come back, but it rarely leads to liver cirrhosis after a transplant.
Read more about liver treatments
Living with PBC
If you’ve been diagnosed with PBC, there are a few things you can do to make yourself feel better.
- Cut down on salt. This will help with fluid retention and swelling
- Cut down on the fat in your diet, especially if you are overweight
- Drink plenty of water
- Cut out alcohol
- Don’t take any drugs that can harm the liver (including illegal drugs, alternative medicines and liver tonics)
- Do more exercise. Walking is great. Try to do some weight training as well to protect your bones
- De-stress if you can
- Stop smoking
- Look after your skin, especially if you are very itchy
- Get your teeth checked regularly, especially if you have a dry mouth
There are things you can do to manage some of the more bothersome symptoms of PBC.
Tiredness
People with PBC often feel very tired. It’s not a sign of how serious the disease is – sometimes people in the early stages feel very tired while others with more advanced disease don’t feel tired at all. To treat tiredness, your doctor will talk to you about your diet, exercise and sleep. They may also test your thyroid as thyroid disease is more common in people with PBC and can also make you tired.
Itching
There are several treatments available to help with itching. These include antihistamines, antibiotics or a medication called cholestyramine (brand name Questran Lite). If you’re itchy, try to keep your fingernails short. Avoid hot baths and showers, try to wear natural fibres and watch you don’t get too much sun.
Dry eyes and mouth
You can buy artificial tears and saliva over-the-counter from a pharmacy. Chewing gum or sucking a lolly can help.
Diet
It’s important to eat a healthy, balanced diet to improve your overall health and help your liver work properly. Because your body may have trouble absorbing some vitamins, your doctor may recommend supplements such as A, D, E and K, calcium, folic acid or iron.
Fluid retention
You may be given diuretics, medications to help your body control fluid.
More Information
There is a peer to peer support group on Facebook for people with a diagnosis of PBC where you can talk to other people living with PBC. It is operated independently of the Liver Foundation.
The PBC Foundation in Canada has some useful resources. Please note that these resources are created for people living in Canada, any advice about specific treatments and treatment pathways may not be relevant for the Australian context.
The PBC Foundation UK has some useful resources. Please note that these resources are created for people living in the United Kingdom, any advice about specific treatments and treatment pathways may not be relevant for the Australian context.
What next?
Read more about living wellReferences
American Liver Foundation. Primary biliary cholangitis (PBC)
Better Health Channel. Primary biliary cirrhosis
British Liver Trust. Primary Biliary Cholangitis (PBC)
French J, van der Mei I, Simpson S Jr, Ng J, Angus P, Lubel J, Nicoll A, Sood S, Roberts SK, Kemp W, Arachchi N, Dev A, Thompson A, Gow PJ. Increasing prevalence of primary biliary cholangitis in Victoria, Australia. J Gastroenterol Hepatol. 2020 Apr;35(4):673-679. doi: 10.1111/jgh.14924. Epub 2019 Dec 28. PMID: 31693755.
Hirschfield GM, Dyson JK, Alexander GJM, Chapman MH, Collier J, Hübscher S, Patanwala I, Pereira SP, Thain C, Thorburn D, Tiniakos D, Walmsley M, Webster G, Jones DEJ. The British Society of Gastroenterology/UK-PBC primary biliary cholangitis treatment and management guidelines. Gut. 2018 Sep;67(9):1568-1594. doi: 10.1136/gutjnl-2017-315259. Epub 2018 Mar 28. PMID: 29593060; PMCID: PMC6109281
Mayo Clinic. Primary biliary cholangitis
MSD Professional Manual. Primary Biliary Cholangitis (PBC)
National Institute of Diabetes and Digestive and Kidney Diseases. Health information; Liver disease; Primary Biliary Cholangitis (Primary Biliary Cirrhosis).
NORD – National Organization for Rare Disorders. Rare Disease Database; Primary Biliary Cholangitis.
Reviewed June 2025
