Primary Sclerosing Cholangitis
Key points
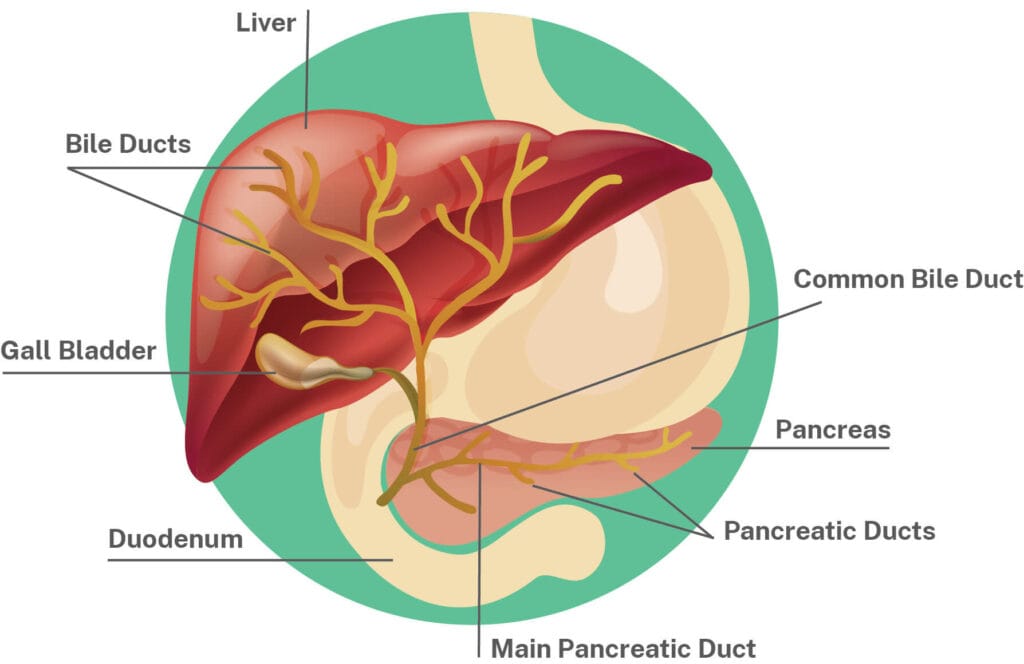
- Primary Sclerosing Cholangitis (PSC) is a condition that affects the bile ducts (the tubes that carry bile from the liver to the gallbladder and then to the intestines)
- Most people who develop PSC also have an inflammatory bowel disease such as ulcerative colitis or Crohn’s disease
- PSC often gets worse over time
- Eventually, it may lead to liver failure, infections or tumours in the bile duct or liver
What is PSC?
Primary Sclerosing Cholangitis (PSC) causes chronic (long lasting) inflammation in the bile ducts inside and outside the liver.
The bile ducts become inflamed and scarred, and eventually blocked. This causes bile to build up in the liver. Bile is the yellow-green liquid that is put out from the liver, stored in the gallbladder and passes into the small intestine to help digest food by breaking down fat.
Too much bile in the liver kills off liver cells and can cause scarring (cirrhosis). Eventually, the liver can’t function anymore.
This in turn can lead to other conditions including:
- Infections – the inflammation in the bile ducts can prevent bile from flowing out of the liver. This can lead to repeated infections, especially in people whose bile ducts are scarred by surgery
- Portal hypertension – the portal vein is the main blood vessel that carries blood into the liver. When blood can’t flow into the liver, pressure builds up in the vein. To relieve pressure in the portal vein, the blood takes detours around the liver in other veins in the oesophagus (food pipe) or stomach. This condition can lead to swelling of the belly (ascites) as fluid leaks out of the of the liver, or swelling in other veins (varices). When veins get swollen they can burst and bleed, which can be life threatening
- Low levels of vitamins A, D, E and K in the body
- Osteoporosis (brittle bones)
- Tumours in the bile ducts (called cholangiocarcinoma) or gallbladder cancer
- Colon cancer if you also have inflammatory bowel disease.
 The disease gets worse very slowly. Some people have PSC for years before they notice symptoms. Once they are diagnosed, it can take 10 to 15 years or more before liver failure develops.
The disease gets worse very slowly. Some people have PSC for years before they notice symptoms. Once they are diagnosed, it can take 10 to 15 years or more before liver failure develops.
Some other rare autoimmune disorders are also more common in people with PSC and in their family members.
PSC in children
PSC is rarer in children. You can watch Professor Winita Hardikar, Liver Foundation Board member and Head of the Liver and Intestinal Transplant Unit at The Royal Children’s Hospital Melbourne deliver a talk about Paediatric PSC here.
What are the symptoms of PSC?
PSC often doesn’t cause any symptoms. People only find out they have PSC because they have a blood test for something else.
If you do have symptoms, at first they might include:
As the disease gets worse, other symptoms may appear such as:
- Belly pain
- Fever and chills and night sweats (from infections)
- Weight loss
- Dark urine (wee)
- Light coloured poos
- Nausea
- Discomfort in the upper abdomen from an enlarged liver or spleen
Symptoms may come and go, or they may get worse over time.
How is PSC diagnosed?
If your doctor thinks you may have PSC, they will take a blood test to look at your liver function. This test looks for raised liver enzymes such as alanine aminotransferase (ALT) or aspartate aminotransferase (AST) (can indicate inflammation), alkaline phosphatase (ALP) or gamma glutamyltransferase (GGT) (can indicate narrowed or blocked bile ducts). The tests will also look for other chemicals that indicate whether your liver is working properly.
You may also have a scan called Magnetic Resonance Cholangiopancreatography (MRCP) to look at your bile ducts. This is a type of MRI scan.
Sometimes a procedure called endoscopic retrograde cholangiopancreatography (ERCP) is used instead of or as well as an MRI. This is done by passing a flexible tube down your throat. Dye is put into the bile duct where it connects with the upper part of your small intestine. X-rays are used during the procedure to track where the dye goes. Narrowed sections of the bile duct may be able to be stretched open to allow the bile to get through.
If it’s still not clear what’s causing the disease, you may need a liver biopsy. This is when a small piece of tissue is removed from the liver to be examined under a microscope.
Read more about liver testsWhy did I get PSC?
It’s not clear why some people develop PSC. It’s thought to be triggered by the immune system reacting abnormally to an infection or a toxin. It’s also likely that you inherit the genes for PSC. The cause of PSC is probably different for different people.
PSC is most common in men aged 30 to 60, and in people with northern European heritage. It seems to be more common in Australia than previously thought. It’s one of the reasons that people need a liver transplant in Australia.
How is PSC treated?
So far there’s no treatment that can slow or reverse the liver damage that’s caused by PSC. Treatments will focus on easing the symptoms and preventing complications.
Medicines you might be given include:
- Ursodeoxycholic acid or UDCA capsules to prevent damage from the build-up of bile
- Cholestyramine or other medications to manage severe itching
Sometimes it is necessary to improve the flow of bile if there is a tight narrowing found at the time of an ERCP procedure. This may involve stretching the narrowing using a balloon (called a dilatation) or inserting a stent into the bile duct to hold it open.
PSC can cause frequent infections, so people with the condition often need to take antibiotics which many mean being admitted to hospital for a short time. They may also need vitamin supplements, as PSC stops the liver from absorbing some vitamins properly.
People with PSC need to be monitored for complications. For example, your doctor may order a bone density scan to check for osteoporosis and a colonoscopy, which looks inside the bowel for disease. These tests are usually needed on a regular basis every one or two years.
Portal hypertension is sometimes treated with a type of medicine called a beta-blocker.
If you develop liver failure, the only treatment is a liver transplant. A liver transplant can cure PSC, but in some people the condition comes back.
Read more about liver treatmentsLiving with PSC
If you’ve been diagnosed with PSC, there are a few things you can do to make yourself feel better.
- Cut out alcohol
- Eat a healthy, balanced diet
- Lose weight if you need to
- Make sure your hepatitis A and B vaccinations are up to date
- Don’t take any drugs that can harm the liver (including illegal drugs, alternative medicines and liver tonics)
- Do more physical activity. Walking is great. Try to do some weight training as well to protect your bones and keep you strong
- De-stress if you can
- Stop smoking
- Look after your skin, especially if you are very itchy
Additional information and support
What next?
Read more about living well
References
American Liver Foundation. Primary sclerosing cholangitis (PSC)
Mayo Clinic. Primary Sclerosing Cholangitis
MSD Professional Manual. Primary Sclerosing Cholangitis (PSC)
NORD – National Organization for Rare Disorders. Rare Disease Information; Primary Sclerosing Cholangitis
PSC Support Australia. What is PSC?
Tan N, Ngu N, Worland T, Lee T, Abrahams T, Pandya K, Freeman E, Hannah N, Gazelakis K, Madden RG, Lynch KD, Valaydon Z, Sood S, Dev A, Bell S, Thompson A, Ding J, Nicoll AJ, Liu K, Gow P, Lubel J, Kemp W, Roberts SK, Majeed A; Melbourne Liver Group. Epidemiology and outcomes of primary sclerosing cholangitis: an Australian multicentre retrospective cohort study. Hepatol Int. 2022 Jun 3. doi: 10.1007/s12072-022-10356-1.
Reviewed November 2022
