Can Liver Damage Be Reversed?
Key points
- Yes, liver damage can be reversed. Your liver can repair itself!
- Making some changes can reverse a lot of liver damage and avoid serious problems in future
- You don’t have to change everything all at once. Small changes can have a big impact.
- To protect your liver:
- eat a balanced diet
- cut down on highly processed foods and drinks (sweets, soft drinks, pizza and chips) and foods that have a lot of sugar
- move more
- look after high blood pressure and cholesterol
- reduce further harm to your liver by not drinking alcohol
- being a healthy weight protects your liver
The liver is an amazing organ. It’s the only organ in the body that can repair itself by creating new tissue. If you take care of it, and make some changes to the way you live, eat and drink, you can reverse a lot of damage and avoid serious complications in the future.
Liver damage happens when there is inflammation, which leads to scarring (fibrosis) and then cirrhosis. This takes many years. The earlier you find the problem and remove the cause of the liver damage, the better the chances of your liver healing.
Sometimes liver damage can be caused by a virus or autoimmune condition. There are effective treatments for these conditions.
It’s never too late. See your doctor and follow a healthy lifestyle to reduce inflammation, reverse scarring and improve how your liver works.
How does liver damage happen?
There are different stages to liver damage.
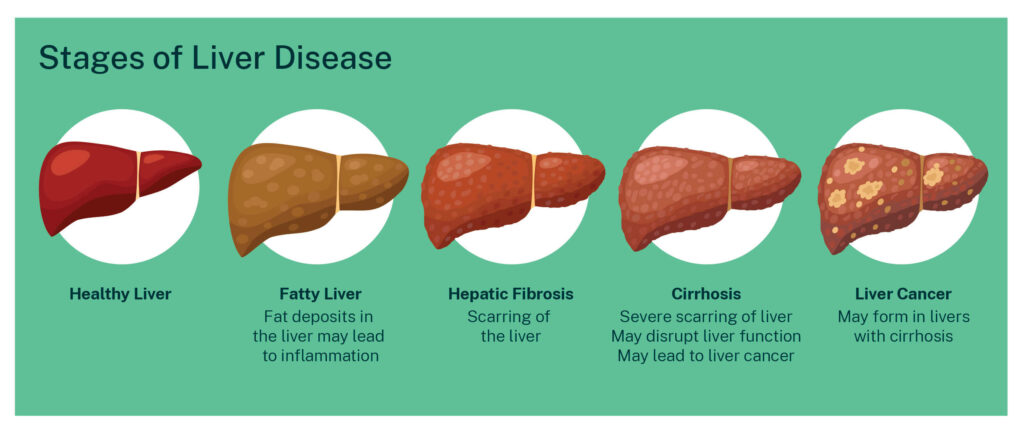
First comes inflammation. This is called hepatitis. It can be caused by many things including viruses, problems with metabolism, drinking too much alcohol, or having an autoimmune condition.
Next comes fibrosis. When the liver is inflamed for a long time, the cells try to repair themselves by producing collagen. This makes the cells in the liver stiffer. Eventually collagen and other proteins build up between the liver cells and make scar tissue. This scarring, or fibrosis, can spread through the liver and stop it from working properly. Fibrosis can be reversed if you address it early enough.
Finally, cirrhosis develops. Cirrhosis means severe scarring of the liver. Even at this stage of liver disease, fixing the underlying condition can reverse cirrhosis and prevent complications like liver failure.
So it’s never too late to make a change. Treating the underlying cause of your liver disease can prevent the damage from getting worse and can reverse the damage that has been done. This may lower your risk of developing liver cancer or liver failure, or of needing a liver transplant in the future.
How can I reverse the damage to my liver?
If you follow your medical team’s instructions and have regular monitoring, you can live a healthy life and potentially reverse some of the damage done to your liver.
The best way to reverse the damage is to remove whatever is causing it.
For example, if you have fatty liver caused by drinking alcohol, it’s important to stop drinking. If it’s caused by your diet or being overweight, then it’s important to eat healthily and lose weight. Liver Foundation has launched The Fatty Liver Diet, a simple, evidence-based guide to eating well and being active for people living with fatty liver disease.
Your doctor will also manage other conditions you might have that can increase the chance of progressing to cirrhosis. For example, if you have hepatitis B or hepatitis C, you may need antiviral medicines. Or if you have problems with your metabolism, you may need medicine to control your cholesterol, high blood pressure or blood sugar levels.
If you have liver disease, it’s very important to see your doctor regularly to check your health and ensure that your liver damage isn’t getting worse.
Read more about lifestyle changes you can make to safeguard your liver health.
Watch Rob’s story – reversing fatty liver disease
Transcript
I was a little bit in shock and a little bit scared. I didn’t really understand how I was living my life and I didn’t realise that the things I was doing were so dangerous to my health.
I’ve been working as a mechanic for probably the last 25 years. It wasn’t really something I ever wanted to do, but kind of fell into it and loved the kind of environment that I found myself in with the people, the kind of workshop vibe.
Growing up in western suburbs, of course, soccer was my number one. I’m a big A.S. Roma fan. Dedicated most of my time to watching games at four in the morning.
I remember the day I was diagnosed with fatty liver. My local GP gave me a call, told me to come in and he showed me that my liver numbers were a little bit too high.
So GP sent me for a couple of other tests and we sat down. I didn’t really know what fatty liver was or how serious it was. He helped me understand that this was actually good news. It was reversible with a couple of simple changes to my lifestyle.
I worked in the music industry, performing live since the early 2000s, where it was an industry that we smoked and we drank a lot. And I thought quitting smoking, replacing that with eating sweets, was a healthier option. And it just gave me a different type of health concern which could potentially be even more dangerous.
I needed to change and I’d had a severe back injury which kept me off work for a year and a half. And at its worst point, I was ordering a lot of fast food.
I decided to change my diet, get to real foods, preparing my meals at home, simplified it. Lots of veggies, lots of good lean proteins, lots of healthy fish, olive oils. I decided to exercise, a lot of resistance training and I focused on healthy relationships in my life and I just took care of myself a little more than I had for the past few years.
With the right support at work, all my workmates, we’ve made some changes, we prepare real foods, lean proteins, healthy vegetables and we enjoy it all together.
So after three months, I went back and did the next round of blood tests with the doctor and he gave me a high five. And he said that the numbers were right within the regular zone that he liked and he was really, really happy and he couldn’t believe that I’d done it so easily.
I was pretty lucky, I found it pretty early. I got really strict, I cut out refined carbs and cut out sugars completely and I felt like the exercise and the training helped me more than anything.
The advice I’d give to anybody who’s been diagnosed with fatty liver is don’t be embarrassed. Like one in three Australians struggle with some form of liver disease.
It’s really normal, it’s not your fault.
Make changes, do it for yourself. Do it for you. You’ll enjoy the changes you make and you’ll be really proud of yourself.
And this time in a week, I’m going to be standing in the middle of the Stadio Olimpico, cheering on Roma instead of being in the hospital somewhere.
What happens when liver damage is very severe?
Sometimes liver disease can become advanced. Someone with advanced liver disease might develop serious complications:
- Fluid build-up in the belly (ascites)
- Yellow skin or eyes (jaundice)
- Confusion (hepatic encephalopathy)
- Internal bleeding
- Liver failure.
But these signs of poor liver function can often be greatly improved by treating the underlying disease and actively preventing or treating any complications.
To do this, your doctor may prescribe medicines. They may also recommend you:
- Avoid all alcohol
- Stop smoking
- Eat a healthy balanced diet
- Get regular exercise
- Go to regular check-ups to monitor your condition and find any complications early.
One complication of advanced liver disease is liver cancer. Having a regular ultrasound scan every 6 months can find early signs of liver cancer, which may be able to be cured.
It is very important that you see your healthcare team regularly and follow all advice. Otherwise, you could be at greater risk of further complications that may be difficult to treat.
In some people with liver failure or early liver cancer, the damage can’t be reversed. A liver transplant may be recommended to give you the best chance of living a good quality life. Your doctor will discuss this option with you if it is felt to be appropriate.
Am I at risk of my liver damage getting worse?
You are at greater risk of liver damage getting worse if:
- You are carrying excess body weight
- You have poorly controlled diabetes
- You continue to smoke or drink alcohol
- You don’t take medication as prescribed
- You don’t make changes to protect your liver health
References
American Liver Foundation. The progression of liver disease.
Francque SM, Marchesini G, Kautz A, Walmsley M, Dorner R, Lazarus JV, Zelber-Sagi S, Hallsworth K, Busetto L, Frühbeck G, Dicker D, Woodward E, Korenjak M, Willemse J, Koek GH, Vinker S, Ungan M, Mendive JM, Lionis C. Non-alcoholic fatty liver disease: A patient guideline. JHEP Rep. 2021 Sep 17;3(5):100322. doi: 10.1016/j.jhepr.2021.100322. PMID: 34693236; PMCID: PMC8514420.
Harrison SA, Fecht W, Brunt EM, Neuschwander-Tetri BA. Orlistat for overweight subjects with nonalcoholic steatohepatitis: A randomized, prospective trial. Hepatology. 2009 Jan;49(1):80-6. doi: 10.1002/hep.22575. PMID: 19053049.
Karanjia RN et al. World J Gastroenterol 2016;22:9880–97. 2. Shiha G, Mousa N. (2020). Chapter 36: Noninvasive Biomarkers for Liver Fibrosis. In: Radu-Ionita F et al. (eds). Liver diseases: a multidisciplinary textbook. Springer International Publishing, Cham, pp 427–442.
Promrat K, Kleiner DE, Niemeier HM, Jackvony E, Kearns M, Wands JR, Fava JL, Wing RR. Randomized controlled trial testing the effects of weight loss on nonalcoholic steatohepatitis. Hepatology. 2010 Jan;51(1):121-9. doi: 10.1002/hep.23276. PMID: 19827166; PMCID: PMC2799538.
Vilar-Gomez E, Martinez-Perez Y, Calzadilla-Bertot L, Torres-Gonzalez A, Gra-Oramas B, Gonzalez-Fabian L, Friedman SL, Diago M, Romero-Gomez M. Weight Loss Through Lifestyle Modification Significantly Reduces Features of Nonalcoholic Steatohepatitis. Gastroenterology. 2015 Aug;149(2):367-78.e5; quiz e14-5. doi: 10.1053/j.gastro.2015.04.005. Epub 2015 Apr 10. PMID: 25865049.
Weisrchen R, Tacke F. Clin Liver Dis (Hoboken) 2016;8(4):94–9.
Wong VW, Chan RS, Wong GL, Cheung BH, Chu WC, Yeung DK, Chim AM, Lai JW, Li LS, Sea MM, Chan FK, Sung JJ, Woo J, Chan HL. Community-based lifestyle modification programme for non-alcoholic fatty liver disease: a randomized controlled trial. J Hepatol. 2013 Sep;59(3):536-42. doi: 10.1016/j.jhep.2013.04.013. Epub 2013 Apr 23. PMID: 23623998.
Reviewed November 2022

